
Polyvagal Theory in Neurodiverse Conditions and Chronic Pain
I recently came across a mention of polyvagal theory and how stimulating the vagus nerve affects the activation of the parasympathetic system, which is responsible for relaxation.
Given that we, neurodivergent individuals, statistically find ourselves in tension more often and suffer from chronic pain, I decided to check out what this beast actually is and how it works) And of course, sensational headlines weren't enough for me - I went looking for evidence-based research and studies. And here's what I found.
What is polyvagal theory
It was developed by neurophysiologist Stephen Porges in 1994. The theory describes how our autonomic nervous system is hierarchically organized through the vagus nerve, and how this affects social behavior, emotions, and physical state. In short, our nervous system has three modes of operation:
- Ventral vagal: "I'm safe, I can relax and recover."
- Sympathetic: "uncertainty / danger, activating mobilization."
- Dorsal vagal: "that's it, I'm shutting down or dissociating."
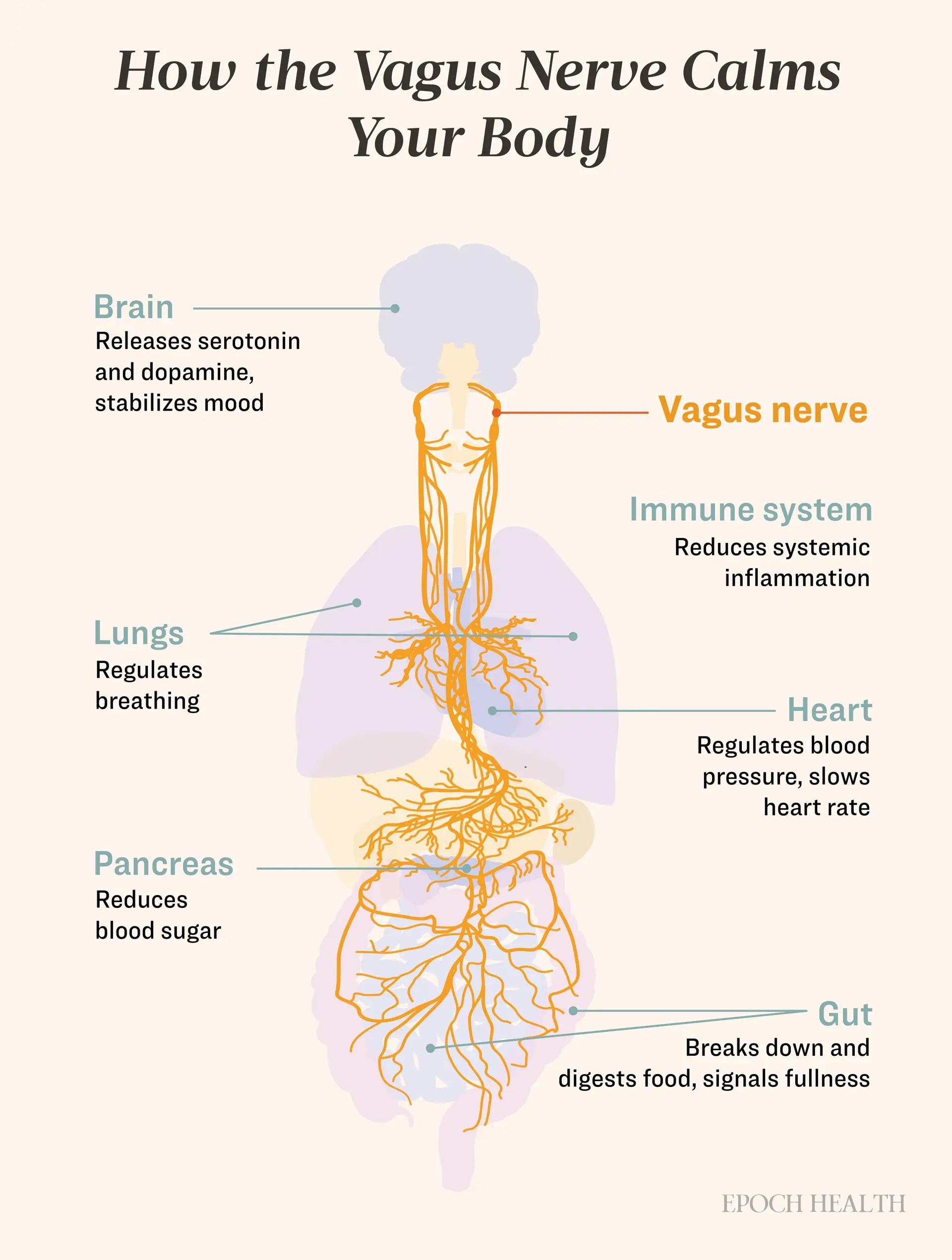
But how does this actually work and what do the heart, gut, and immune system have to do with it
Here we need to talk about the insula, a small brain region that acts as a dispatcher between the body and the brain. Interoception - is the ability to read signals from within: heartbeat, breathing, pressure in the intestines. The vagus nerve carries these signals upward → brainstem (nucleus of the solitary tract, NTS) → thalamus → posterior insular cortex. It's the posterior region that receives raw interoceptive signals - temperature, pain, pressure, organ state. This is the "primary sensory cortex of the body."
Next comes processing: from the posterior region, the signal moves forward to the middle, then to the anterior insular cortex. There, the raw sensation transforms into subjective experience: "I feel bad," "I'm anxious," "something's wrong." The anterior region integrates this with emotions, memory, and context.
Top-down: it's precisely the anterior insular cortex together with the anterior cingulate gyrus that sends regulatory signals back through the autonomic nervous system to the organs. And this is where things get really interesting.
Autistic people have been found to have reduced activity in the anterior insular cortex - the region responsible for integrating body signals with emotional experience. In other words: the brain receives a fuzzy picture from inside the body and begins to interpret it. And the brain often interprets anything imprecise and unclear as potential danger.
And then here's what happens next. When the brain perceives a signal as dangerous, even if there's no real threat, it activates the HPA axis (hypothalamus - pituitary - adrenal glands) and the sympathetic nervous system. This is accompanied by the release of pro-inflammatory cytokines - interleukin-1β, interleukin-6, tumor necrosis factor.
That is, inflammation is triggered not by the threat itself, but by how the brain interprets it.
Sympathetic projections to lymphoid tissue: bone marrow, lymph nodes, spleen can trigger immune responses in response to real or perceived environmental threats. When the nervous system is chronically stuck in a state of anxiety, as it is for many of us, this immune response becomes background. Constant. This is where chronic inflammation with no apparent cause comes from, heart rate problems, digestive issues, breathing problems. Psychosomatics in its concrete action.
So what does this have to do with us, neurodivergent people
And here's where things get really interesting. Research documents in autistic people a sustained sympathetic hyperactivation, i.e., the nervous system chronically operates in mobilization mode.
With ADHD, the nervous system constantly oscillates between hypoactivation (brain fog, fatigue, boredom) and hyperactivation (impulsivity, anxiety). Boredom for an ADHD brain is literally a stress signal, because the nervous system doesn't know how to relax in silence. That's why we need stimulation so much: a TV show or podcast in the background, crafts, drawing, puzzles, etc.
Now about chronic pain
A 2023 study with a sample of 448 adults showed: autistic traits are statistically associated with chronic musculoskeletal pain, fibromyalgia, irritable bowel syndrome and migraines, and all of this is partially mediated by autonomic nervous system dysfunction.
In another study, 21% of autistic adults had a diagnosed central sensitization syndrome, and more than 40% of people with pronounced autistic traits had fibromyalgia. And this is not hypochondria, but a nervous system that cannot relax.
So what about the vagus nerve
Vagus nerve stimulation increases parasympathetic activity and has shown potential in treating depression, anxiety, and chronic pain. But an important nuance: most clinical research was about electrical stimulation with devices. Auricular vagus nerve stimulation is being studied as a non-pharmacological method for chronic and acute pain and results are encouraging. Breathing, vocalization, cold water on the face - these techniques have physiological justification.
Where the theory is controversial
Some researchers from the autistic community rightly point out: the idea that autism is a ventral vagus deficit that needs to be "fixed." No, autism is a polygenic innate condition, literally a somewhat different structure and connectivity in certain brain regions. And vagus nerve stimulation won't cure it.
The specific anatomical premises of polyvagal theory, especially regarding the uniqueness of the ventral branch in mammals, are disputed in neurobiology. This doesn't mean the entire theory is garbage. It means the mechanism is more complex than a pretty three-level diagram. Real phenomena: autonomic dysregulation, interoception, the connection between the nervous system and inflammation exist and are proven independently of whether polyvagal theory is right about anatomical details.
What you can try right now
Remember: this is not treatment, not a substitute for therapy. These are tools with physiological justification:
- Extended exhale. An exhale longer than the inhale is direct parasympathetic activation. The scheme couldn't be simpler: inhale for 4 counts, exhale for 8. I often do this myself when I feel I'm revving up too much.
- Cold water on the face or wrists. Sounds like grandma's advice, but the mechanism is real - the diving reflex sharply lowers heart rate through the vagus nerve.
- Vocalization. Humming, buzzing, singing anything. The vagus nerve innervates the vocal cords, vibration stimulates it. This is one reason why auditory stimming works so well.
- If you want to go deeper, in Russian there are two translated books from Multimethod publishing: Stephen Porges "Polyvagal Theory. Neurophysiological Foundations of Emotions, Attachment, Communication and Self-Regulation" - this is the primary source, but academic. Deb Dana "Polyvagal Theory in Psychotherapy": more practical, about how it works in live therapy. If you just want practice with explanations, there's also "Tuning the Body-Brain System" by Linehardt, Schmidt-Fetzer and Cobb. That very book about vagus nerve exercises. Mechanisms are explained clearly there, exercises are simple. Evidence base is partial, but the authors don't promise to fix everything, and that's already good.Links to sources: Polyvagal theory - the foundation
- Porges S.W. Polyvagal Theory: Current Status, Clinical Applications, and Future Directions. Clinical Neuropsychiatry, 2025. https://pmc.ncbi.nlm.nih.gov/articles/PMC12302812/
- Autonomic dysregulation in autism Autonomic Dysfunction in Autism Spectrum Disorder. PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC8756818/
- ADHD and the nervous system Why Polyvagal Theory Makes So Much Sense for ADHD, Autism, and AuDHD. Myndset Therapeutics, 2025. https://www.myndset-therapeutics.com/post/why-polyvagal-theory-makes-so-much-sense-for-adhd-autism-and-audhd
- Chronic pain and autistic traits Ryan et al. Autistic Traits Correlate with Chronic Musculoskeletal Pain. OBM Neurobiology, 2023. https://www.lidsen.com/journals/neurobiology/neurobiology-07-01-155
- Fibromyalgia and autism Ward et al. Increased rates of chronic physical health conditions in autistic adolescents and adults. Molecular Autism, 2023.
- Vagus nerve stimulation for pain Duff et al. Clinical Efficacy of Auricular Vagus Nerve Stimulation. Pain Therapy, 2024. https://link.springer.com/article/10.1007/s40122-024-00657-8
- Insular cortex, interoception and immunity Koren & Rolls. Immunoception: the insular cortex perspective. Cellular & Molecular Immunology, 2023. https://www.nature.com/articles/s41423-023-01051-8
- Anxiety, brain and inflammation - top-down mechanism Muscatell et al. Exaggerated neurobiological sensitivity to threat links anxiety with inflammation. PMC, 2015. https://pmc.ncbi.nlm.nih.gov/articles/PMC4361087/
- Interoception and inflammation in psychiatric disorders Interoception and Inflammation in Psychiatric Disorders. PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC5995132/
- Insular cortex in autism The anterior insula in autism: Under-connected and under-examined. PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC2743776/